Liver Transplantation in the United States
Liver transplantation is a life-saving surgery for persons with acute and chronic liver diseases. In the United States, the major disorders that may result in consideration for liver transplantation include acute liver failure, chronic liver disease with advanced cirrhosis, hepatocellular carcinoma (HCC), and liver-based metabolic defects.[1,2] In the United States, in 2022 there were 9,257 liver transplants performed.[2] From 1988 through 2022, the overall trend was a steady increase in the number of liver transplants performed in the United States, with a 50% increase in transplants during the years 2012 (Figure 1).[2,3,4] Advances in the field of transplantation have improved post-primary liver transplant survival rates in the United States to 91.8% at 1 year after liver transplantation, 83.3% at 3 years, and 76.1% at 5 years.[5,6] This review will discuss general information and principles regarding liver transplantation, with a focus on specific information related to liver transplantation for persons with hepatitis C virus (HCV)
Liver Transplantation in Persons with Chronic HCV Infection
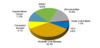
For more than a decade, chronic HCV infection was the most common indication for liver transplantation in the United States, but alcohol-related liver disease is now a more common indication than chronic HCV (Figure 2).[3,7,8] This change reflects both the rise in alcohol-related liver disease and the effectiveness of direct-acting antiviral (DAA) drugs to treat HCV. In the early DAA era, the number of people on the waiting list due to HCV-related complications decreased by 32% in the United States.[9] Since acute HCV rarely causes liver failure, nearly all transplants related to HCV involve persons with chronic HCV infection who have developed cirrhosis-related complications. Data from 2012-2014 for persons with chronic HCV monoinfection who received a liver transplant in the United States showed that most recipients were male (70.8%) and White (69.1%).[10] During this time period, among the 41,557 persons listed for orthotopic liver transplantation, 21,064 (51.2%) received a liver transplant.[10]
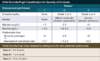
 Elbasvir-Grazoprevir Zepatier
Elbasvir-Grazoprevir Zepatier Glecaprevir-Pibrentasvir Mavyret
Glecaprevir-Pibrentasvir Mavyret Ledipasvir-Sofosbuvir Harvoni
Ledipasvir-Sofosbuvir Harvoni Ribavirin Copegus, Rebetol, Ribasphere
Ribavirin Copegus, Rebetol, Ribasphere Sofosbuvir Sovaldi
Sofosbuvir Sovaldi Sofosbuvir-Velpatasvir Epclusa
Sofosbuvir-Velpatasvir Epclusa Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi
Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi