Hepatitis C virus (HCV) is primarily spread through blood-to-blood contact (parenteral transmission), with injection drug use being the most common risk factor for HCV acquisition. Sexual transmission and perinatal transmission of HCV can occur, but are less common. The following lesson reviews details about HCV transmission risk and emphasizes important prevention messages for persons living with and at risk for HCV.
- Module 1 Overview
Screening and Diagnosis of Hepatitis C Infection - 0%Lesson 1
HCV Epidemiology in the United StatesActivities- 0%Lesson 2
Recommendations for Hepatitis C ScreeningActivities- 0%Lesson 3
Hepatitis C Diagnostic TestingLesson 4. Counseling for Prevention of HCV Transmission
Learning Objective Performance Indicators
- List common routes of HCV transmission
- Discuss appropriate counseling to prevent sexual transmission of HCV
- Describe counseling messages to prevent transmission of HCV through injection drug use
- Explain prevention messages for preventing household transmission of HCV
- Summarize counseling messages for preventing perinatal HCV transmission
Last Updated: January 2nd, 2024Authors:Maria A. Corcorran, MD, MPH,Maria A. Corcorran, MD, MPH
Assistant Professor
Division of Allergy & Infectious Diseases
University of WashingtonH. Nina Kim, MD, MScH. Nina Kim, MD, MSc
Professor of Medicine
Division of Allergy & Infectious Diseases
University of WashingtonDisclosures: Grant to institution: Gilead SciencesReviewer:David H. Spach, MDDavid H. Spach, MD
Professor of Medicine
Division of Allergy & Infectious Diseases
University of WashingtonDisclosures: NoneTable of ContentsIntroduction
Sexual Transmission of HCV
Persons at Risk
Transmission of hepatitis C virus (HCV) through heterosexual contact appears to be uncommon, with early studies showing transmission among long-term monogamous heterosexual partners occurring in less than 1% of couples per year.[1,2,3,4] In a more recent large cross-sectional study of persons with HCV and their partners, investigators estimated a maximum incidence rate of 0.07% per year among monogamous heterosexual couples, which corresponded to approximately one transmission per 190,000 sexual contacts.[5] This risk increases slightly among persons who have multiple sex partners.[6] Multiple reports have identified clusters of acute hepatitis C infection among men who have sex with men (MSM), primarily MSM who have HIV infection.[7,8,9,10,11] When comparing the risk of HCV acquisition among MSM with or without HIV, the risk is significantly higher among MSM who have HIV.[12] It also appears that MSM taking HIV preexposure prophylaxis (PrEP) have an increased risk of acquiring HCV.[13,14] Further, recent cohort studies have also shown a high rate of HCV reinfection among MSM living with HIV, with the risk of reinfection associated with ongoing sexual practices and/or injection drug use.[15,16,17,18]
Factors Associated with Increased Risk of Sexual Transmission
For heterosexuals, having multiple sex partners has been associated with an increased risk of HCV acquisition.[6] Investigators have identified multiple risk factors associated with sexual transmission of HCV among MSM:[12,18]
- Coinfection with HIV
- Unprotected anal intercourse, especially as the receptive partner
- Inconsistent condom use
- Use of recreational drugs, particularly use of drugs during sex
- Recent or concurrent sexually transmitted infections
- Multiple casual or anonymous sex partners
- Group sex
- Certain sex practices that result in rectal bleeding or damage to the rectal mucosa, including fisting and sharing sex toys.
Prevention
The Centers for Disease Control and Prevention (CDC) recommends the following for preventing the sexual transmission of HCV.[19]
- Persons with HCV who have one long-term steady sex partner do not need to alter their sex practices. Long-term partners should be offered the option of receiving HCV counseling and undergoing HCV testing.
- For HCV-serodifferent couples attempting to minimizing the risk of HCV transmission, using latex condoms and avoiding sex practices that potentially result in bleeding should presumably further reduce the risk of sexual HCV transmission.
- Individuals with known hepatitis C should be counseled to disclose their HCV status to their sex partners.
- Persons with HCV who have multiple sex partners should consistently use condoms during sexual activity to reduce their risk of transmitting HCV to their partners and to reduce the risk of transmission or acquisition of other sexually transmitted diseases, including HIV and hepatitis B virus.
- Given the significant potential risk of sexual transmission of HCV among MSM, particularly MSM with HIV, it is important for medical providers and persons with HCV to discuss sex and drug use practices known to increase the risk of transmitting HCV. Individuals should also be counseled that reinfection with hepatitis C can occur and be offered counseling on safer sex and drug use practices that reduce the risk for reinfection.
- For persons with HIV and HCV coinfection who are taking HIV antiretroviral therapy and have consistently undetectable HIV RNA levels, their risk of HIV transmission is negligible, but they need to be reminded that HIV antiretroviral therapy will not impact their risk of transmitting HCV to others.
Injection Drug Use and HCV Transmission
HCV Infection among Persons Who Inject Drugs
Hepatitis C virus is transmitted very efficiently by the parenteral route, and injection drug use is the most commonly reported risk factor for new cases of HCV in the United States.[20,21,22] Reported cases of acute hepatitis C infection in the United States rose annually from 2010 to 2021, with an overall increase of 492% during that time period.[22,23,24] New infections occurred more often in persons aged 30 through 39 years of age, American Indian/Alaska Native or White persons, and those residing in non-urban areas, particularly in Appalachia, the Midwest, and New England.[24,25,26,27] Among persons who inject drugs (PWID), approximately 50% acquire HCV within 5 years of the first time they inject drugs.[28] The prevalence of a positive HCV antibody test among persons who inject drugs is as high as 65-80% in certain geographic locations, and has been shown to increase with age, number of years of injecting, and frequency of injecting.[29,30,31] After spontaneous clearance or successful treatment, PWID can experience HCV reinfection, although the rate of reinfection appears to be lower than the incident rate of infection among PWID.[32,33,34]
Risk Factors for HCV Transmission in Injection Drug Use
The risk of HCV transmission among PWID is clearly associated with the sharing of syringes and needles. In addition, multiple studies have demonstrated the role of sharing equipment used to prepare and inject drugs, including filtration cottons, drug cookers, and rinse water, in HCV acquisition.[35,36] Persons should receive counseling to avoid sharing needles, syringes, and any drug preparation equipment, including the prepared drug itself (Figure 1). Laboratory studies suggest that HCV can persist for prolonged periods of time in contaminated syringes, particularly in syringes with a larger residual volume (tuberculin syringes) versus low void volume syringes (insulin syringes). It is estimated that HCV can survive outside the body at room temperature for up to 3 weeks; the survival of HCV is longer in liquids than in dried substances, and survival is longer at lower temperatures.[37,38,39] In addition, the survival of HCV in syringes depends on the design of the syringe needle and the dead space volume.[40,41,42]
Prevention
The following counseling information is intended for persons without HCV who are at risk of acquiring hepatitis C infection and persons with HCV who are at risk of transmitting HCV to others. In addition, persons should receive counseling regarding available syringe service programs and medications for opioid use disorder (e.g., buprenorphine and methadone).[43,44,45,46,47] See the North American Syringe Exchange Network (NASEN) website for harm reduction locations in the United States. Individuals with HCV who have been cured of hepatitis C with treatment should also be counseled that reinfection with HCV is possible and prevention strategies should be used on a long-term basis.[48,49,50] The following summarizes key strategies to share with persons who inject drugs to help reduce the acquisition or transmission of HCV:[19]
- Reduce the frequency of injecting
- Use new, sterile needles and syringes each time you inject
- Do not share or reuse needles or syringes following use
- Safely dispose of needles and syringes
- Do not share or reuse other injection materials, including cookers, cottons, water, and drugs
- Receive substance use treatment and support for safe injection practices
Household HCV Transmission
Potential for Household HCV Transmission
Although HCV is transmitted most efficiently through the parenteral route, some epidemiologic studies have shown household contacts of HCV seropositive patients to have a slightly elevated risk of HCV infection.[51,52,53] Confounding factors include the potential for shared parenteral exposures, such as medical or dental procedures and injections; sexual exposure between partners and spouses; and vertical transmission between mother and infant. Thus it is difficult to quantify the risk associated with nonsexual, household only exposures to HCV. A systematic review of this found an increased risk for HCV infection in siblings and household contacts of persons living with chronic HCV infection.[54] The increased risk for HCV infection in families and spouses included in the controlled studies correlated with the severity of liver disease in the index patient, the number of family members infected with HCV, the duration of exposure to the index patient, and sexual contact with the index patient.[53] Additional domestic risk factors for HCV transmission identified in uncontrolled studies were sharing razors and nail clippers between family members and patients, reuse of syringes, and coinfection with HIV.[53]
Prevention
Although the risk of isolated intra-household, nonsexual transmission is very low, persons living with HCV should be counseled on strategies to reduce potential transmission to any household contact. The CDC recommends that persons with HCV infection should receive the following precautions and information regarding potential household transmission of HCV:[19]
- Avoid sharing razors, shaving equipment, toothbrushes, dental equipment, nail clippers, or other personal care items that contain any trace of blood.
- Cover cuts or sores on the skin to keep from spreading infectious blood.
- HCV can survive outside the body for at least several days, so any blood spill (including dried blood) should be cleaned up using a dilution of one part household bleach to 10 parts water by a person wearing gloves during the entire cleanup.
- HCV is not spread through food, water, eating utensils, or casual contact (such as sneezing, coughing, touching, hugging).
- Routine testing for nonsexual household contacts of persons with HCV is not recommended unless a history exists of a direct (percutaneous or mucosal) exposure to blood.
Perinatal HCV Transmission
Risk of Perinatal HCV Transmission
Perinatal (mother-to-child) transmission of hepatitis C occurs in approximately 5 to 6% of pregnant women with HCV who have viremia, a rate significantly lower than with perinatal transmission of hepatitis B or HIV.[55,56,57,58,59] The timing of perinatal HCV transmission is poorly understood, but intrauterine, intrapartum, and postnatal transmission are possible, with the majority of infants likely becoming infected late in utero (Figure 2).[58,59] In a systematic review of 77 studies published between 1990 and 2000, investigators calculated a 4.3% rate of mother-to-infant transmission among women with HCV viremia.[55] A 2014 systematic review and meta-analysis of 109 articles reported a 5.8% risk of perinatal HCV transmission among women who were HCV RNA positive, whereas a more recent 2023 study estimated a vertical transmission of HCV to be 7.2% among HIV-seronegative mothers with HCV without HIV coinfection and 12.1% among those with HCV and HIV coinfection.[58,59]
Risk Factors for Perinatal HCV Transmission
The most important risk factors associated with an increased risk of mother-to-child HCV transmission include HIV coinfection of the mother and detectable HCV viremia during pregnancy.[55,60,61] Based on multiple studies, coinfection with HIV approximately doubles the risk of vertical HCV transmission (10.8% versus 5.8%).[58,59] In general, studies suggest that the risk of vertical transmission is correlated with a higher maternal HCV viral load, and mothers who are HCV antibody-positive but RNA-negative are felt to have a negligible risk of vertical transmission.[62,63,64] Other identified risk factors include female gender of the infant; prolonged rupture of membranes (longer than 6 hours); obstetric procedures and intrapartum events that lead to infant exposure to maternal blood infected with HCV, such as internal fetal monitoring or vaginal/perineal lacerations; and maternal injection drug use.[60,62,65] In contrast, mother-to-child HCV transmission has not been associated with the mode of delivery (vaginal versus Cesarean birth) or breastfeeding.[56,60] Data from large cohorts of mothers with HCV infection and their exposed infants demonstrate that safe breastfeeding (e.g., breastfeeding in the absence of damaged, cracked, or bleeding nipples) does not increase the rate of perinatal transmission of HCV.[66]
Prevention of Mother-to-Child HCV Transmission
For pregnant women with HCV infection, there are no interventions or prophylactic measures that have been demonstrated to prevent perinatal transmission of HCV. The direct-acting antiviral medications to treat HCV in adults have not been adequately studied in pregnancy or in breastfeeding women. Thus, treatment of HCV during pregnancy is not routinely recommended as a strategy to prevent vertical HCV transmission. Pregnant women with HCV infection should be counseled on the low (approximately 6%) risk potential for HCV transmission to their baby. They should also be counseled on the need for ongoing follow-up and testing for themselves and their child; mothers with HCV also need follow-up for potential spontaneous HCV clearance, as up to 10% of women spontaneously clear HCV after childbirth.[67,68,69]
Recommendations
The following summary recommendations are based on guidance from the CDC and the Association for the Study of Liver Diseases and Infectious Diseases Society of America (AASLD-IDSA):[7,70,71,72]
- Universal screening of all pregnant women for HCV infection is recommended.
- For women of childbearing age with known HCV infection, treatment of HCV with direct-acting antiviral therapy is recommended prior to considering pregnancy, if this is practical and feasible. If HCV treatment is curative and given prior to conception, it will virtually eliminate the subsequent risk of vertical HCV transmission.
- Treatment of HCV during pregnancy is not routinely recommended at this time but can be considered on an individualized basis.
- Pregnant women with chronic HCV should undergo evaluation of liver function and liver disease severity based on laboratory evaluation; women with cirrhosis should receive counseling about the potential complications in pregnancy for both mother and child.
- The decision to perform an elective cesarean section should not be based on the HCV infection status of the mother, as currently available data does not support performing a cesarean section to reduce perinatal HCV transmission.
- Breastfeeding in the absence of damaged, cracked, or bleeding nipples is felt to be safe for mothers with HCV infection. Most experts recommend temporarily stopping breastfeeding if the mother has cracking or bleeding in the nipple or surrounding areola. During this time, the mother should use a breast pump to express and discard her milk. Once the nipple region has healed, the mother can resume breastfeeding.
- Infants born to mothers with HCV infection should be tested for HCV infection. This should be done via HCV RNA testing of the infant at age 2 to 6 months.
- Women with HCV should have HCV RNA values performed at approximately 9 to 12 months after giving birth to assess for possible spontaneous HCV clearance.
Summary Points
- The risk of heterosexual transmission of HCV is low. Persons with HCV infection who are in long-term monogamous relationships should be advised they do not need to alter their sexual practices based on HCV infection.
- Sexual transmission of HCV can occur among MSM, and the risk may be substantial with sexual practices that result in bleeding or damage to rectal mucosal tissue; this risk is significantly higher among MSM with HIV.
- Men who have sex with men and who have HCV should receive counseling regarding the potential sexual transmission of HCV to others and should be advised to use condoms and avoid rough sex.
- Hepatitis C is transmitted efficiently via injection drug use and transmission can occur when sharing needles, syringes, or other equipment used to prepare and inject drugs, and through sexual contact.
- Persons with HCV and injection drug use should receive counseling regarding available resources for syringe services and treatment for opioid use disorder, as well as assistance with measures to reduce the risk of transmission if they continue to inject drugs.
- Reinfection of HCV infection can occur and persons who have spontaneous resolution of HCV or cure through treatment should be counseled on the risk of reinfection.
- Household transmission of HCV (not related to sexual or injection drug transmission) can rarely occur. Persons living in a household with any individual who has HCV infection should be advised not to share razors, toothbrushes, or nail clippers.
- Mother-to-child HCV transmission occurs in approximately 6% of pregnant women with HCV infection; the risk of infection is not significantly altered by the mode of delivery or by breastfeeding.
- Women with HCV do not need to avoid pregnancy, nor do they need to avoid breastfeeding.
- Infants born to mothers with HCV infection should have follow-up for evaluation of possible HCV infection.
Citations
- 1.Terrault NA. Sexual activity as a risk factor for hepatitis C. Hepatology. 2002;36(5 Suppl 1):S99-105.[PubMed Abstract] -
- 2.Kao JH, Liu CJ, Chen PJ, Chen W, Lai MY, Chen DS. Low incidence of hepatitis C virus transmission between spouses: a prospective study. J Gastroenterol Hepatol. 2000;15:391-5.[PubMed Abstract] -
- 3.Tahan V, Karaca C, Yildirim B, et al. Sexual transmission of HCV between spouses. Am J Gastroenterol. 2005;100:821-4.[PubMed Abstract] -
- 4.Vandelli C, Renzo F, Romanò L, et al. Lack of evidence of sexual transmission of hepatitis C among monogamous couples: results of a 10-year prospective follow-up study. Am J Gastroenterol. 2004;99:855-9.[PubMed Abstract] -
- 5.Terrault NA, Dodge JL, Murphy EL, Tavis JE, Kiss A, Levin TR, Gish RG, Busch MP, Reingold AL, Alter MJ. Sexual transmission of hepatitis C virus among monogamous heterosexual couples: the HCV partners study. Hepatology. 2013;57:881-9.[PubMed Abstract] -
- 6.Tohme RA, Holmberg SD. Is sexual contact a major mode of hepatitis C virus transmission? Hepatology. 2010;52:1497-505.[PubMed Abstract] -
- 7.Centers for Disease Control and Prevention (CDC). Sexual transmission of hepatitis C virus among HIV-infected men who have sex with men--New York City, 2005-2010. MMWR Morb Mortal Wkly Rep. 2011;60:945-50.[PubMed Abstract] -
- 8.Hoornenborg E, Achterbergh RCA, Schim van der Loeff MF, et al. MSM starting preexposure prophylaxis are at risk of hepatitis C virus infection. AIDS. 2017;31:1603-1610.[PubMed Abstract] -
- 9.Jin F, Matthews GV, Grulich AE. Sexual transmission of hepatitis C virus among gay and bisexual men: a systematic review. Sex Health. 2017;14:28-41.[PubMed Abstract] -
- 10.Urbanus AT, Van De Laar TJ, Geskus R, et al. Trends in hepatitis C virus infections among MSM attending a sexually transmitted infection clinic; 1995-2010. AIDS. 2014;28:781-90.[PubMed Abstract] -
- 11.van de Laar TJ, Matthews GV, Prins M, Danta M. Acute hepatitis C in HIV-infected men who have sex with men: an emerging sexually transmitted infection. AIDS. 2010;24:1799-812.[PubMed Abstract] -
- 12.Gorgos L. Sexual transmission of viral hepatitis. Infect Dis Clin North Am. 2013;27:811-36.[PubMed Abstract] -
- 13.Ramière C, Charre C, Miailhes P, et al. Patterns of Hepatitis C Virus Transmission in Human Immunodeficiency Virus (HIV)-infected and HIV-negative Men Who Have Sex With Men. Clin Infect Dis. 2019;69:2127-35.[PubMed Abstract] -
- 14.Jin F, Dore GJ, Matthews G, et al. Prevalence and incidence of hepatitis C virus infection in men who have sex with men: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2021;6:39-56.[PubMed Abstract] -
- 15.Young J, Rossi C, Gill J, et al. Risk Factors for Hepatitis C Virus Reinfection After Sustained Virologic Response in Patients Coinfected With HIV. Clin Infect Dis. 2017;64:1154-1162.[PubMed Abstract] -
- 16.Martin TC, Martin NK, Hickman M, et al. Hepatitis C virus reinfection incidence and treatment outcome among HIV-positive MSM. AIDS. 2013;27:2551-7.[PubMed Abstract] -
- 17.Ingiliz P, Martin TC, Rodger A, et al. HCV reinfection incidence and spontaneous clearance rates in HIV-positive men who have sex with men in Western Europe. J Hepatol. 2017;66:282-287.[PubMed Abstract] -
- 18.Newsum AM, Matser A, Schinkel J, et al. Incidence of HCV reinfection among HIV-positive MSM and its association with sexual risk behavior: a longitudinal analysis. Clin Infect Dis. 2020 May 27. Online ahead of print.[PubMed Abstract] -
- 19.Recommendations for the prevention and control of hepatitis C virus (HCV) infection and HCV-related chronic disease. Centers for Disease Control. MMWR Recomm Rep. 1998;47(RR-19):1-39.[CDC and MMWR] -
- 20.Page K, Hahn JA, Evans J, et al. Acute hepatitis C virus infection in young adult injection drug users: a prospective study of incident infection, resolution, and reinfection. J Infect Dis. 2009;200:1216-26.[PubMed Abstract] -
- 21.Alter MJ. Prevention of spread of hepatitis C. Hepatology. 2002;36(5 Suppl 1):S93-8.[PubMed Abstract] -
- 22.Centers for Disease Control and Prevention (CDC). 2019 Viral Hepatitis Surveillance Report—Hepatitis C. Published May 2021.[CDC] -
- 23.Centers for Disease Control and Prevention (CDC). Viral Hepatitis Statistics and Surveillance—United States, 2016.
- 24.Centers for Disease Control and Prevention (CDC). Hepatitis C Surveillance 2021. Published August 2023.[CDC] -
- 25.Suryaprasad AG, White JZ, Xu F, et al. Emerging epidemic of hepatitis C virus infections among young nonurban persons who inject drugs in the United States, 2006-2012. Clin Infect Dis. 2014;59:1411-9.[PubMed Abstract] -
- 26.Zibbell JE, Asher AK, Patel RC, et al. Increases in Acute Hepatitis C Virus Infection Related to a Growing Opioid Epidemic and Associated Injection Drug Use, United States, 2004 to 2014. Am J Public Health. 2018;108:175-181.[PubMed Abstract] -
- 27.Zibbell JE, Iqbal K, Patel RC, et al. Increases in hepatitis C virus infection related to injection drug use among persons aged ≤30 years - Kentucky, Tennessee, Virginia, and West Virginia, 2006-2012. MMWR Morb Mortal Wkly Rep. 2015;64:453-8.[PubMed Abstract] -
- 28.Hagan H, Pouget ER, Des Jarlais DC, Lelutiu-Weinberger C. Meta-regression of hepatitis C virus infection in relation to time since onset of illicit drug injection: the influence of time and place. Am J Epidemiol. 2008;168:1099-109.[PubMed Abstract] -
- 29.Corcorran MA, Tsui JI, Scott JD, Dombrowski JC, Glick SN. Age and gender-specific hepatitis C continuum of care and predictors of direct acting antiviral treatment among persons who inject drugs in Seattle, Washington. Drug Alcohol Depend. 2021;220:108525.[PubMed Abstract] -
- 30.Nelson PK, Mathers BM, Cowie B, et al. Global epidemiology of hepatitis B and hepatitis C in people who inject drugs: results of systematic reviews. Lancet. 2011;378:571-83.[PubMed Abstract] -
- 31.Ozga JE, Syvertsen JL, Pollini RA. Hepatitis C antibody prevalence, correlates and barriers to care among people who inject drugs in Central California. J Viral Hepat. 2022;29:518-28.[PubMed Abstract] -
- 32.AASLD-IDSA. HCV Guidance: Recommendations for testing, management, and treating hepatitis C. Key populations: identification and management of HCV in people who inject drugs.
- 33.Hajarizadeh B, Cunningham EB, Valerio H, et al. Hepatitis C reinfection after successful antiviral treatment among people who inject drugs: A meta-analysis. J Hepatol. 2020;72:643-57.[PubMed Abstract] -
- 34.Muller A, Vlahov D, Akiyama MJ, Kurth A. Hepatitis C Reinfection in People Who Inject Drugs in Resource-Limited Countries: A Systematic Review and Analysis. Int J Environ Res Public Health. 2020;17:4951.[PubMed Abstract] -
- 35.Hahn JA, Page-Shafer K, Lum PJ, et al. Hepatitis C virus seroconversion among young injection drug users: relationships and risks. J Infect Dis. 2002;186:1558-64. [PubMed Abstract] -
- 36.Hagan H, Pouget ER, Williams IT, et al. Attribution of hepatitis C virus seroconversion risk in young injection drug users in 5 US cities. J Infect Dis. 2010;201:378-85.[PubMed Abstract] -
- 37.Doerrbecker J, Friesland M, Ciesek S, et al. Inactivation and survival of hepatitis C virus on inanimate surfaces. J Infect Dis. 2011;204:1830-8.[PubMed Abstract] -
- 38.Paintsil E, Binka M, Patel A, Lindenbach BD, Heimer R. Hepatitis C virus maintains infectivity for weeks after drying on inanimate surfaces at room temperature: implications for risks of transmission. J Infect Dis. 2014;209:1205-11.[PubMed Abstract] -
- 39.Song H, Li J, Shi S, Yan L, Zhuang H, Li K. Thermal stability and inactivation of hepatitis C virus grown in cell culture. Virol J. 2010;7:40.[PubMed Abstract] -
- 40.Paintsil E, He H, Peters C, Lindenbach BD, Heimer R. Survival of hepatitis C virus in syringes: implication for transmission among injection drug users. J Infect Dis. 2010;202:984-90. [PubMed Abstract] -
- 41.Zule WA, Pande PG, Otiashvili D, et al. Options for reducing HIV transmission related to the dead space in needles and syringes. Harm Reduct J. 2018;15:3.[PubMed Abstract] -
- 42.Binka M, Paintsil E, Patel A, Lindenbach BD, Heimer R. Survival of Hepatitis C Virus in Syringes Is Dependent on the Design of the Syringe-Needle and Dead Space Volume. PLoS One. 2015;10:e0139737.[PubMed Abstract] -
- 43.Tsui JI, Evans JL, Lum PJ, Hahn JA, Page K. Association of opioid agonist therapy with lower incidence of hepatitis C virus infection in young adult injection drug users. JAMA Intern Med. 2014;174:1974-81.[PubMed Abstract] -
- 44.Nolan S, Dias Lima V, Fairbairn N, et al. The impact of methadone maintenance therapy on hepatitis C incidence among illicit drug users. Addiction. 2014;109:2053-9.[PubMed Abstract] -
- 45.Hagan H, Pouget ER, Des Jarlais DC. A systematic review and meta-analysis of interventions to prevent hepatitis C virus infection in people who inject drugs. J Infect Dis. 2011;204:74-83. [PubMed Abstract] -
- 46.Platt L, Minozzi S, Reed J, et al. Needle syringe programmes and opioid substitution therapy for preventing hepatitis C transmission in people who inject drugs. Cochrane Database Syst Rev. 2017;9:CD012021.[PubMed Abstract] -
- 47.Turner KM, Hutchinson S, Vickerman P, et al. The impact of needle and syringe provision and opiate substitution therapy on the incidence of hepatitis C virus in injecting drug users: pooling of UK evidence. Addiction. 2011;106:1978-88.[PubMed Abstract] -
- 48.Falade-Nwulia O, Sulkowski MS, Merkow A, Latkin C, Mehta SH. Understanding and addressing hepatitis C reinfection in the oral direct-acting antiviral era. J Viral Hepat. 2018;25:220-227.[PubMed Abstract] -
- 49.Grady BP, Schinkel J, Thomas XV, Dalgard O. Hepatitis C virus reinfection following treatment among people who use drugs. Clin Infect Dis. 2013;57 Suppl 2:S105-10.[PubMed Abstract] -
- 50.Martinello M, Hajarizadeh B, Grebely J, Dore GJ, Matthews GV. HCV Cure and Reinfection Among People With HIV/HCV Coinfection and People Who Inject Drugs. Curr HIV/AIDS Rep. 2017;14:110-121.[PubMed Abstract] -
- 51.Diago M, Zapater R, Tuset C, et al. Intrafamily transmission of hepatitis C virus: sexual and non-sexual contacts. J Hepatol. 1996;25:125-8.[PubMed Abstract] -
- 52.Omar MZ, Metwally MA, El-Feky HM, Ahmed IA, Ismail MA, Idris A. Role of intrafamilial transmission in high prevalence of hepatitis C virus in Egypt. Hepat Med. 2017;9:27-33.[PubMed Abstract] -
- 53.Indolfi G, Nesi A, Resti M. Intrafamilial transmission of hepatitis C virus. J Med Virol. 2013;85:608-14.[PubMed Abstract] -
- 54.Ackerman Z, Ackerman E, Paltiel O. Intrafamilial transmission of hepatitis C virus: a systematic review. J Viral Hepat. 2000;7:93-103. [PubMed Abstract] -
- 55.Yeung LT, King SM, Roberts EA. Mother-to-infant transmission of hepatitis C virus. Hepatology. 2001;34:223-9.[PubMed Abstract] -
- 56.Post JJ. Update on hepatitis C and implications for pregnancy. Obstet Med. 2017;10:157-160.[PubMed Abstract] -
- 57.Page CM, Hughes BL, Rhee EHJ, Kuller JA. Hepatitis C in Pregnancy: Review of Current Knowledge and Updated Recommendations for Management. Obstet Gynecol Surv. 2017;72:347-355.[PubMed Abstract] -
- 58.Benova L, Mohamoud YA, Calvert C, Abu-Raddad LJ. Vertical transmission of hepatitis C virus: systematic review and meta-analysis. Clin Infect Dis. 2014;59:765-73.[PubMed Abstract] -
- 59.Ades AE, Gordon F, Scott K, et al. Overall Vertical Transmission of Hepatitis C Virus, Transmission Net of Clearance, and Timing of Transmission. Clin Infect Dis. 2023;76:905-12.[PubMed Abstract] -
- 60.European Paediatric Hepatitis C Virus Network. A significant sex--but not elective cesarean section--effect on mother-to-child transmission of hepatitis C virus infection. J Infect Dis. 2005;192:1872-9.[PubMed Abstract] -
- 61.Roberts EA, Yeung L. Maternal-infant transmission of hepatitis C virus infection. Hepatology. 2002;36:S106-13.[PubMed Abstract] -
- 62.Mast EE, Hwang LY, Seto DS, Nolte FS, Nainan OV, Wurtzel H, Alter MJ. Risk factors for perinatal transmission of hepatitis C virus (HCV) and the natural history of HCV infection acquired in infancy. J Infect Dis. 2005;192:1880-9.[PubMed Abstract] -
- 63.Ohto H, Terazawa S, Sasaki N, et al. Transmission of hepatitis C virus from mothers to infants. The Vertical Transmission of Hepatitis C Virus Collaborative Study Group. N Engl J Med. 1994;330:744-50.[PubMed Abstract] -
- 64.Ceci O, Margiotta M, Marello F, et al. Vertical transmission of hepatitis C virus in a cohort of 2,447 HIV-seronegative pregnant women: a 24-month prospective study. J Pediatr Gastroenterol Nutr. 2001;33:570-5.[PubMed Abstract] -
- 65.Resti M, Azzari C, Galli L, et al. Maternal drug use is a preeminent risk factor for mother-to-child hepatitis C virus transmission: results from a multicenter study of 1372 mother-infant pairs. J Infect Dis. 2002;185:567-72.[PubMed Abstract] -
- 66.Cottrell EB, Chou R, Wasson N, Rahman B, Guise JM. Reducing risk for mother-to-infant transmission of hepatitis C virus: a systematic review for the U.S. Preventive Services Task Force. Ann Intern Med. 2013;158:109-13.[PubMed Abstract] -
- 67.Hashem M, Jhaveri R, Saleh DA, et al. Spontaneous Viral Load Decline and Subsequent Clearance of Chronic Hepatitis C Virus in Postpartum Women Correlates With Favorable Interleukin-28B Gene Allele. Clin Infect Dis. 2017;65:999-1005.[PubMed Abstract] -
- 68.Hattori Y, Orito E, Ohno T, et al. Loss of hepatitis C virus RNA after parturition in female patients with chronic HCV infection. J Med Virol. 2003;71:205-11.[PubMed Abstract] -
- 69.Lin HH, Kao JH. Hepatitis C virus load during pregnancy and puerperium. BJOG. 2000;107:1503-6.[PubMed Abstract] -
- 70.AASLD-IDSA. HCV Guidance: Recommendations for testing, management, and treating hepatitis C. Unique populations: HCV in pregnancy
- 71.Centers for Disease Control and Prevention (CDC). National Notifiable Diseases Surveillance System (NNDSS). Hepatitis C, Perinatal Infection: 2018 Case Definition.[CDC and NNDSS] -
- 72.Panagiotakopoulos L, Sandul AL, Conners EE, Foster MA, Nelson NP, Wester C. CDC Recommendations for Hepatitis C Testing Among Perinatally Exposed Infants and Children - United States, 2023. MMWR Recomm Rep. 2023;72:1-21.[PubMed Abstract] -
Additional References
- Bradshaw D1, Matthews G, Danta M. Sexually transmitted hepatitis C infection: the new epidemic in MSM? Curr Opin Infect Dis. 2013;26:66-72.[PubMed Abstract] -
- Foster AL, Gaisa MM, Hijdra RM, et al. Shedding of Hepatitis C Virus Into the Rectum of HIV-infected Men Who Have Sex With Men. Clin Infect Dis. 2017;64:284-288.[PubMed Abstract] -
- Kuncio DE, Newbern EC, Johnson CC, Viner KM. Failure to Test and Identify Perinatally Infected Children Born to Hepatitis C Virus-Infected Women. Clin Infect Dis. 2016;62:980-5.[PubMed Abstract] -
- Ly KN, Jiles RB, Teshale EH, Foster MA, Pesano RL, Holmberg SD. Hepatitis C Virus Infection Among Reproductive-Aged Women and Children in the United States, 2006 to 2014. Ann Intern Med. 2017;166:775-782.[PubMed Abstract] -
- Pufall EL, Kall M, Shahmanesh M, et al. Sexualized drug use ('chemsex') and high-risk sexual behaviours in HIV-positive men who have sex with men. HIV Med. 2018;19:261-270.[PubMed Abstract] -
- Sarrazin C, Isakov V, Svarovskaia ES, et al. Late Relapse Versus Hepatitis C Virus Reinfection in Patients With Sustained Virologic Response After Sofosbuvir-Based Therapies. Clin Infect Dis. 2017;64:44-52.[PubMed Abstract] -
- Schillie S, Wester C, Osborne M, Wesolowski L, Ryerson AB. CDC Recommendations for Hepatitis C Screening Among Adults - United States, 2020. MMWR Recomm Rep. 2020;69:1-17.[PubMed Abstract] -
- Simmons B, Saleem J, Hill A, Riley RD, Cooke GS. Risk of Late Relapse or Reinfection With Hepatitis C Virus After Achieving a Sustained Virological Response: A Systematic Review and Meta-analysis. Clin Infect Dis. 2016;62:683-94.[PubMed Abstract] -
- US Preventive Services Task Force, Owens DK, Davidson KW, et al. Screening for Hepatitis C Virus Infection in Adolescents and Adults: US Preventive Services Task Force Recommendation Statement. JAMA. 2020;323:970-5.[PubMed Abstract] -
- Watts T, Stockman L, Martin J, Guilfoyle S, Vergeront JM. Increased Risk for Mother-to-Infant Transmission of Hepatitis C Virus Among Medicaid Recipients - Wisconsin, 2011-2015. MMWR Morb Mortal Wkly Rep. 2017;66:1136-1139.[PubMed Abstract] -
- Yaphe S, Bozinoff N, Kyle R, Shivkumar S, Pai NP, Klein M. Incidence of acute hepatitis C virus infection among men who have sex with men with and without HIV infection: a systematic review. Sex Transm Infect. 2012;88:558-64.[PubMed Abstract] -
Figures
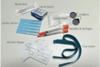 Figure 1. Injection Drug WorksPhotograph of injection equipment courtesy of the Hepatitis Education Project
Figure 1. Injection Drug WorksPhotograph of injection equipment courtesy of the Hepatitis Education Project Figure 2. Timing of Vertical Hepatitis C TransmissionSource: Ades AE, Gordon F, Scott K, et al. Overall Vertical Transmission of Hepatitis C Virus, Transmission Net of Clearance, and Timing of Transmission. Clin Infect Dis. 2023;76:905-12.
Figure 2. Timing of Vertical Hepatitis C TransmissionSource: Ades AE, Gordon F, Scott K, et al. Overall Vertical Transmission of Hepatitis C Virus, Transmission Net of Clearance, and Timing of Transmission. Clin Infect Dis. 2023;76:905-12.Share by e-mail
Check
-On-
Learning
QuestionsThe Check-on-Learning Questions are short and topic related. They are meant to help you stay on track throughout each lesson and check your understanding of key concepts.You must be signed in to customize your interaction with these questions.
- 0%Lesson 2
Since you've received 80% or better on this quiz, you may claim continuing education credit.
You seem to have a popup blocker enabled. If you want to skip this dialog please Always allow popup windows for the online course.
 Elbasvir-Grazoprevir Zepatier
Elbasvir-Grazoprevir Zepatier Glecaprevir-Pibrentasvir Mavyret
Glecaprevir-Pibrentasvir Mavyret Ledipasvir-Sofosbuvir Harvoni
Ledipasvir-Sofosbuvir Harvoni Ribavirin Copegus, Rebetol, Ribasphere
Ribavirin Copegus, Rebetol, Ribasphere Sofosbuvir Sovaldi
Sofosbuvir Sovaldi Sofosbuvir-Velpatasvir Epclusa
Sofosbuvir-Velpatasvir Epclusa Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi
Sofosbuvir-Velpatasvir-Voxilaprevir Vosevi
